Urinary Tract Infections: Causes, Antibiotics, and Prevention
Every year, about 8 million people in the U.S. visit a doctor because of a urinary tract infection (UTI). It’s one of the most common infections you can get-especially if you’re a woman. But even though it’s common, it’s not something to ignore. Left untreated, a simple bladder infection can turn into a kidney infection, or worse, sepsis. The good news? We know a lot about what causes UTIs, how to treat them, and how to stop them from coming back.
What Actually Causes a UTI?
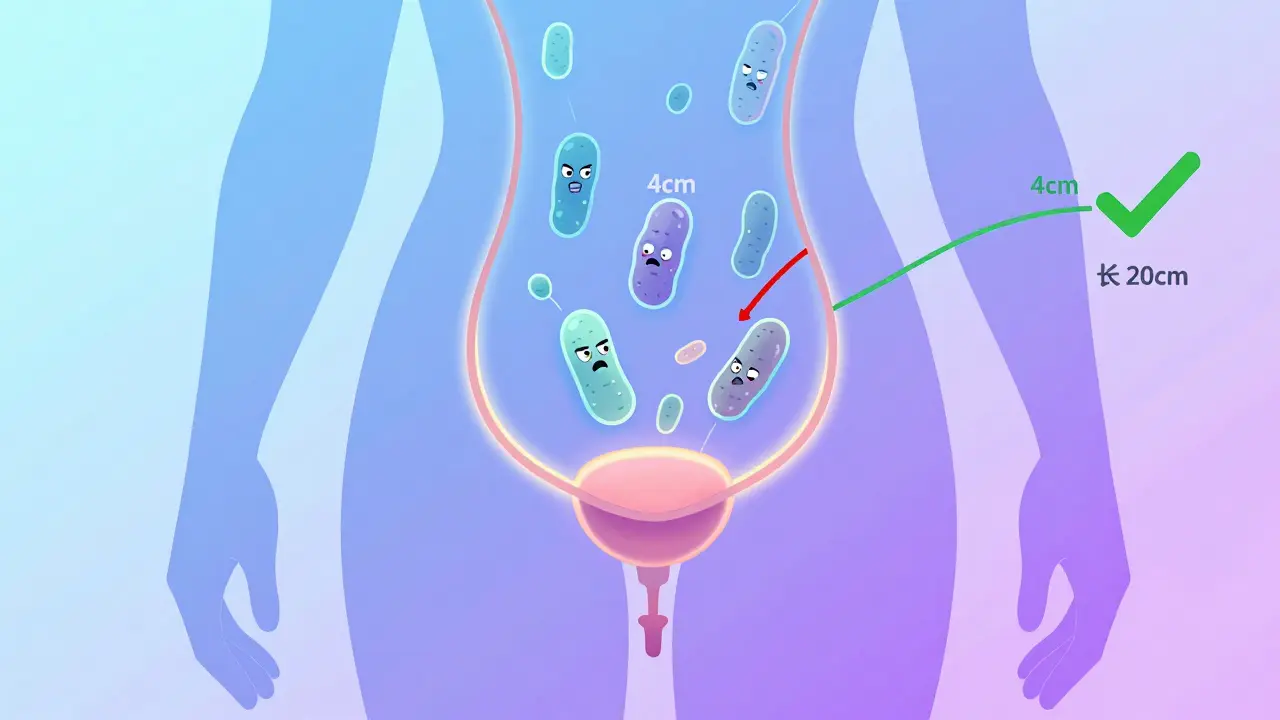
Most UTIs start with bacteria. Not just any bacteria-Escherichia coli, or E. coli, is responsible for 75% to 95% of all uncomplicated cases. This bacteria lives harmlessly in your gut, but if it gets near your urethra, things go wrong. Women are far more likely to get UTIs than men. Why? Because their urethra is much shorter-about 4 centimeters long-compared to men’s 20 centimeters. That means bacteria have a much shorter trip to the bladder. Other bacteria like Klebsiella, Proteus, and Enterococcus can also cause UTIs, especially in people who’ve been in the hospital or use catheters. These are called complicated UTIs. They’re harder to treat because the bacteria are often resistant to common antibiotics. It’s not just about bacteria. Certain habits make UTIs more likely. Spermicides (like nonoxynol-9) can irritate the skin around the urethra and kill off good bacteria that normally keep bad ones in check. That’s why women who use spermicide-based birth control have 2.5 times higher risk of UTIs. Holding in urine for too long, not drinking enough water, and wiping from back to front after using the toilet also raise your chances.How Do You Know You Have a UTI?
Symptoms are pretty clear if you’ve had one before. For a bladder infection (cystitis), you’ll likely feel:- Burning when you pee (reported by 92% of patients)
- Needing to go often, even if only a drop comes out
- A sudden, strong urge to pee (urgency)
- Pressure or pain in your lower belly
- Cloudy or bloody urine
- Flank pain (sharp pain on one side of your back)
- Fever over 38.3°C (101°F)
- Chills
- Nausea or vomiting
Which Antibiotics Actually Work?
Not all antibiotics are equal when it comes to UTIs. The right one depends on your health, where you live, and what bacteria are common in your area. For a simple bladder infection in a healthy woman, doctors usually start with one of three:- Nitrofurantoin (100 mg twice a day for 5 days) - works in 90% of cases. It’s concentrated in the urine, so it’s great for the bladder. But it won’t reach the kidneys, so don’t use it if you think you have pyelonephritis.
- Trimethoprim-sulfamethoxazole (Bactrim, 160/800 mg twice a day for 3 days) - still effective in places where resistance is below 20%. But in many parts of the U.S., over 30% of E. coli strains are resistant to it now.
- Fosfomycin (3g single dose) - convenient, one-time pill. About 86% effective. Good for people who can’t take other antibiotics.
- Ciprofloxacin (500 mg twice daily for 7-14 days)
- Ceftriaxone (given as an IV shot, then maybe switched to oral pills)

What About Antibiotic Resistance?
This is the big worry. Over the last 10 years, E. coli resistance to common UTI drugs has climbed. In some areas, more than half of infections don’t respond to trimethoprim-sulfamethoxazole. That’s why doctors are moving away from one-size-fits-all treatment. In places like Boston, where resistance is high, nitrofurantoin or fosfomycin are now first-line choices. In rural areas with lower resistance, Bactrim might still work fine. That’s why testing urine (urine culture) matters-especially if you’ve had multiple UTIs or if your symptoms don’t improve. New antibiotics are coming. In 2024, the FDA approved gepotidacin, the first new UTI drug in 20 years. It works against resistant strains and showed 92% cure rates in trials. It’s not widely available yet, but it’s a sign we’re finally making progress.How to Prevent UTIs-For Good
Prevention is way better than treatment. Here’s what actually works, backed by science:- Drink at least 1.5 liters of water a day. A 2022 JAMA study showed this cuts UTI risk by 48%. Water flushes bacteria out before they settle in.
- Pee after sex. This reduces UTI risk by about 50%. Don’t wait-go right after.
- Avoid spermicides. If you use them for birth control, switch to condoms without spermicide, a diaphragm, or another method.
- Wipe front to back. This one sounds basic, but it’s often done wrong. Always wipe from the urethra toward the anus, not the other way around.
- Postcoital prophylaxis - Take a single dose of nitrofurantoin (50-100 mg) or trimethoprim (100 mg) within 2 hours after sex. This cuts recurrence by 95% in clinical trials.
- Low-dose daily antibiotics - Taking nitrofurantoin 50 mg or trimethoprim 100 mg every night can reduce episodes from nearly 7 per year to less than 1. Used for 6-12 months, then stopped.
- Vaginal estrogen - For postmenopausal women, applying a small amount of estrogen cream (0.5g) twice a week reduces UTIs by 70%. Estrogen helps restore healthy vaginal bacteria that block E. coli.
What About Cranberry and D-Mannose?
Cranberry juice? Probably not. Most commercial juices have too little of the active ingredient-proanthocyanidins (PACs). But supplements with at least 36mg of PACs daily can reduce UTIs by 39% in women with frequent infections, according to a 2022 Cochrane review. Even better: D-mannose. It’s a natural sugar that binds to E. coli, stopping it from sticking to the bladder wall. A 2021 study in European Urology found D-mannose (2g daily) was 83% effective at preventing recurrence-better than antibiotics in that study. It’s safe, doesn’t kill good bacteria, and costs less than most antibiotics.
What Doesn’t Work?
A lot of things you hear about don’t hold up:- Drinking vinegar or lemon water - no proof.
- Using antibacterial wipes daily - can irritate skin and make things worse.
- Over-the-counter pain relievers like AZO (phenazopyridine) - they numb the burning but don’t treat the infection. Don’t rely on them to hide symptoms.
When to See a Doctor
If you have symptoms of a UTI, don’t wait. Most people feel better within 48 hours of starting the right antibiotic. But if:- Your symptoms don’t improve in 2 days
- You have fever, back pain, or vomiting
- You’ve had 3 or more UTIs in a year
- You’re pregnant
Final Thoughts
UTIs aren’t glamorous, but they’re common, treatable, and preventable. The key is knowing the facts: E. coli is the main culprit, antibiotics need to match the bug, and prevention beats repetition. Drink water. Pee after sex. Avoid spermicides. Consider D-mannose or vaginal estrogen if you’re prone to recurrences. And if something feels off-don’t brush it off. A simple infection today can become a serious problem tomorrow.Can a UTI go away on its own without antibiotics?
Yes, in some cases. Studies show that 25% to 43% of uncomplicated UTIs in healthy women resolve without antibiotics. But this isn’t a gamble. If you’re young, healthy, and have mild symptoms, you might wait 24-48 hours while drinking plenty of water. But if you’re pregnant, diabetic, over 65, have a fever, or your symptoms worsen, antibiotics are necessary. Untreated UTIs can spread to the kidneys or bloodstream, which can be life-threatening.
Why do I keep getting UTIs even after treatment?
Recurrent UTIs usually mean one of three things: 1) The infection wasn’t fully cleared (sometimes antibiotics don’t reach all the bacteria), 2) You’re being reinfected (often from sexual activity or poor hygiene habits), or 3) There’s an underlying issue like bladder prolapse, kidney stones, or diabetes. Women with recurrent UTIs should see a urologist. Tests like a pelvic exam, ultrasound, or cystoscopy may be needed to rule out structural problems.
Is cranberry juice good for preventing UTIs?
Most cranberry juice isn’t strong enough. The active ingredient, proanthocyanidins (PACs), needs to be in high doses-around 36mg daily-to have any effect. A glass of juice typically has less than 5mg. Supplements with standardized PACs can help reduce recurrence by about 39%, but only in people who get frequent UTIs. Don’t rely on juice as a treatment or prevention method.
Can men get UTIs?
Yes, but it’s rare. Men have longer urethras, which makes it harder for bacteria to reach the bladder. When men do get UTIs, it’s often linked to an underlying problem like an enlarged prostate, kidney stones, or a catheter. A UTI in a man should always be evaluated by a doctor-it’s rarely just a simple infection.
What’s the best way to prevent UTIs after menopause?
Vaginal estrogen therapy is the most effective option. After menopause, estrogen levels drop, which changes the vaginal pH and reduces protective Lactobacillus bacteria. This lets E. coli take over. Applying low-dose vaginal estrogen cream (0.5g) twice a week restores the natural barrier and reduces UTIs by 70%. It’s safe for most women and doesn’t increase cancer risk at this dose.
Do at-home UTI test strips work?
They can help, but they’re not perfect. Tests like AZO Strips detect nitrites and white blood cells in urine-signs of infection. But they miss about 20-30% of UTIs, especially early ones. A negative result doesn’t rule out infection. If you have symptoms but a negative test, still see a doctor. A lab urine culture is the gold standard.

Srividhya Srinivasan
Let me just say this: the fact that we're still relying on 1950s-era antibiotics like nitrofurantoin while Big Pharma sits on golden goose drugs like gepotidacin is a national disgrace. Who approved this? Who let this happen? The FDA is a revolving door for pharmaceutical lobbyists, and we're all paying the price-literally, with our kidneys! And don't even get me started on D-mannose being sold as a 'supplement'-it's a miracle cure, but they won't let you market it as medicine because it can't be patented! CONSPIRACY? NO. IT'S JUST BUSINESS.
Prathamesh Ghodke
Hey, this is actually super helpful! I've had three UTIs in two years, and honestly? I thought cranberry juice was the magic bullet. Turns out, I was just drinking sugary soda with a hint of tartness. Switched to D-mannose powder (2g/day) and haven't had one in 8 months. Also, peeing after sex? Game-changer. I used to think it was just a myth-turns out, science is real. Thanks for the clarity!
Stephen Habegger
Great breakdown. I'm a nurse, and I see this every week. The biggest mistake? People wait too long. They pop AZO, drink lemon water, and pray. But UTIs don't care about your willpower. If you're burning, peeing every 10 minutes, and feel like you're about to explode-go to urgent care. Five minutes. One pill. Back to life. Don't be a hero.
Justin Archuletta
YES! D-mannose is a lifesaver!! I used to be on antibiotics every 3 months. Now? I take 1.5g daily. No side effects. No yeast infections. No drama. And it's cheaper than my coffee habit. Also-stop wiping back to front. I know you think it's 'easier,' but your butt is not a toilet brush. Just. Stop.
Sanjana Rajan
Wow. Just... wow. You're telling me we've been lied to about cranberry juice for decades? And now we're supposed to believe a sugar called D-mannose is better than antibiotics? Sounds like another wellness scam. Also, vaginal estrogen? That's just hormone replacement in disguise. Who's really benefiting from this? Big Pharma? The gynecologists? Someone's making bank off our bladder anxiety.
Kyle Young
It's fascinating how we've reduced a complex biological interaction-bacterial colonization, mucosal immunity, urinary flow, microbiome ecology-to a checklist of 'do this, avoid that.' But what if the root issue isn't hygiene or antibiotics at all? What if our modern diets, chronic dehydration, and environmental toxins have altered our urogenital microbiome so profoundly that even perfect hygiene can't prevent recurrence? Are we treating symptoms-or just masking a systemic failure?
Aileen Nasywa Shabira
Oh, so now we're supposed to believe that peeing after sex prevents UTIs? How convenient. That's the same logic that says 'washing hands prevents germs'-and yet, we still have pandemics. And who decided that '25% of UTIs resolve on their own' is acceptable? That's like saying '25% of car crashes fix themselves.' Why aren't we demanding a vaccine? Why are we just giving women more pills and creams? This feels like a gendered medical neglect dressed up as science.
Kendrick Heyward
I've had 11 UTIs in 3 years. 11. And every time I go to the doctor, they act like I'm being dramatic. Like I'm overreacting. Like it's just 'a girl thing.' I cried in the waiting room last time. I just wanted someone to say, 'I'm sorry this is happening to you.' And now you're telling me to use estrogen cream? I'm 32. I don't want to feel like I'm menopausal. This system is broken. I'm tired. 😭
lawanna major
The science here is remarkably well-structured and evidence-based. I appreciate the nuanced distinction between uncomplicated and complicated UTIs, and the emphasis on antibiotic stewardship. The inclusion of recent data on gepotidacin and D-mannose reflects a commendable alignment with current clinical guidelines. Moreover, the rejection of pseudoscientific remedies like vinegar or antibacterial wipes is both necessary and refreshing. This is precisely the kind of clear, authoritative communication that counters medical misinformation.
Ryan Voeltner
Thank you for this comprehensive overview. It is both informative and respectfully presented. The integration of epidemiological data with practical clinical recommendations demonstrates a high standard of medical communication. I believe such resources are essential in empowering patients to engage meaningfully with their healthcare providers. The emphasis on prevention over reactive treatment is particularly commendable.
Linda Olsson
Let's be real-this whole UTI narrative is just a ploy to sell more antibiotics and supplements. D-mannose? Vaginal estrogen? Who even came up with this? It sounds like a cult. And why are they targeting women specifically? Because we're easier to scare into buying stuff. I've never had a UTI. Never. And I don't pee after sex. I don't drink 1.5L of water. I eat sugar. I use spermicide. And yet? I'm fine. So maybe the real problem isn't bacteria... it's fear.
Ayan Khan
As someone from a culture where urinary health is rarely discussed openly, this post feels revolutionary. In my community, women suffer in silence because it's 'embarrassing.' But here, we have data, solutions, and compassion. I will share this with my sister, my aunt, my colleagues. Knowledge is power. And this is power given freely. Thank you for speaking plainly. We need more of this.
Stephen Habegger
Also, to the person who said 'I've never had a UTI and I do everything wrong'-congrats. You're statistically lucky. But don't mistake luck for wisdom. One day, your body's luck runs out. And then you'll be the one begging for a 3-day course of nitrofurantoin at 3 a.m. with a fever. Don't be that person.