Methotrexate and NSAIDs: Managing Renal Toxicity and Drug Levels
MTX & NSAID Interaction Risk Evaluator
Select an NSAID to check interaction:
Please select an NSAID above to see the risk assessment based on your clinical profile.
Mixing Methotrexate is a dihydrofolate reductase inhibitor used to treat rheumatoid arthritis and various cancers. Also known as MTX, it's a powerful tool, but it has a tricky relationship with a common group of painkillers: Non-Steroidal Anti-Inflammatory Drugs (NSAIDs). While taking an ibuprofen for a headache might seem harmless, doing so while on methotrexate can actually slow down how fast your body gets rid of the medication, potentially leading to dangerous toxicity levels in your blood.
The core problem is that both these drugs rely on your kidneys. When you take an NSAID, it can reduce the blood flow to your kidneys, which in turn makes it harder for your body to flush out methotrexate. For most people on low doses, this is a manageable risk, but for those with existing kidney issues or those on high-dose cancer regimens, it can be a life-threatening combination. Understanding this interaction is about finding the balance between managing pain and keeping your organs safe.
How the Interaction Actually Works
To understand why this happens, we have to look at how the kidneys filter blood. NSAIDs, such as ibuprofen, naproxen, and diclofenac, work by blocking enzymes called COX-1 and COX-2. While this stops pain, it also inhibits the synthesis of renal prostaglandins. Think of these prostaglandins as the "gatekeepers" that keep the blood vessels in your kidneys open. When they are blocked, renal perfusion drops-sometimes by as much as 15-20%.
Because methotrexate is primarily eliminated through the kidneys, this drop in blood flow creates a bottleneck. Pharmacokinetic data shows that NSAIDs can decrease methotrexate and NSAIDs interaction clearance by 25-40%. Additionally, some NSAIDs compete for the same "transport vehicles" (organic anion transporters) in the kidney tubules, essentially pushing the methotrexate back into the bloodstream. There's also the issue of protein binding; some studies show NSAIDs can displace methotrexate from blood proteins, increasing the amount of "free" active drug in your system by up to 30%.
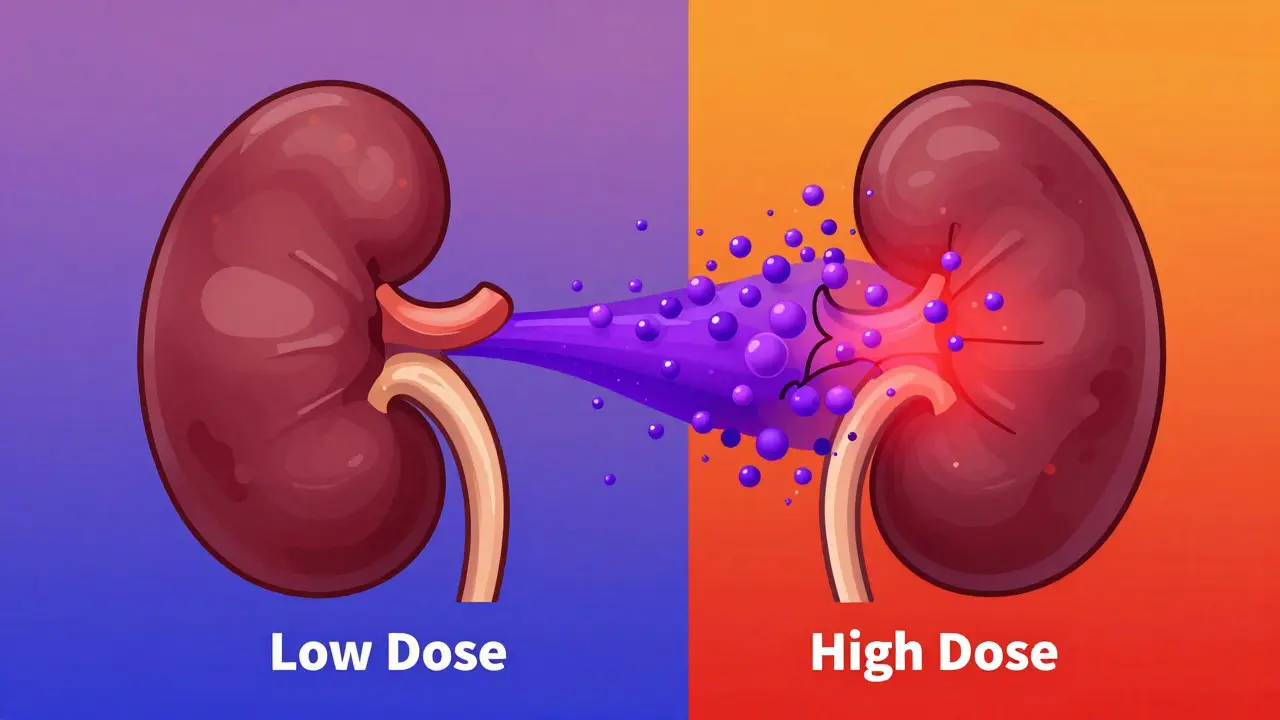
Comparing Risk Levels: Low-Dose vs. High-Dose
Not every patient faces the same level of danger. The risk profile changes dramatically depending on whether you are treating an autoimmune condition or fighting cancer.
For those taking low-dose methotrexate (usually 5-25 mg weekly for rheumatoid arthritis), the risk is generally low if your kidneys are healthy. A large study of over 4,000 patients found no significant increase in adverse events for those with normal renal function (eGFR over 60). However, if your kidney function is already impaired, the risk of complications jumps significantly.
High-dose therapy (typically used in oncology, where doses exceed 15 mg/m²) is a different story. In this scenario, the risk of severe toxicity-including acute kidney injury and myelosuppression (where your bone marrow stops making enough blood cells)-increases nearly five-fold when combined with NSAIDs. This is why oncologists are incredibly strict about avoiding these painkillers during high-dose cycles.
| NSAID Type | Estimated Increase in MTX Levels | Risk Category | Key Note |
|---|---|---|---|
| Ketorolac | Up to 50% | High | Potent prostaglandin inhibitor |
| Ibuprofen | 25-30% | Intermediate | Commonly used, requires monitoring |
| Celecoxib | 10-15% | Low | Selective COX-2 inhibitor |
Warning Signs of Methotrexate Toxicity
Because renal impairment is often "silent," you might not know there is a problem until the drug levels have already spiked. Many patients don't feel anything until their blood counts drop. If you are taking both medications, keep a close eye out for these red flags:
- Extreme Fatigue: Not just being tired, but a crushing exhaustion that doesn't go away with rest.
- Mouth Ulcers: Painful sores in the mouth or throat are a classic sign of folate depletion and drug accumulation.
- Nausea and Vomiting: Sudden gastrointestinal distress shortly after starting an NSAID.
- Easy Bruising or Infections: This suggests your white blood cell or platelet counts have dropped (myelosuppression).
Real-world reports from patient communities highlight the danger of neglecting kidney checks. One patient reported developing severe nausea and a dangerously low white blood cell count (1.8 × 10⁹/L) just three days after starting naproxen without a prior creatinine test. This underscores why "just taking a pill" can be risky when your internal chemistry is already altered by a DMARD.
How to Manage the Interaction Safely
You don't necessarily have to avoid all painkillers, but you do need a strategy. Medical guidelines, including those from the American College of Rheumatology, suggest a few concrete steps to minimize risk.
First, the dose and duration matter. If you must use an NSAID, use the lowest effective dose for the shortest time possible. Second, timing is key. Try to space out your methotrexate dose and your NSAID intake by at least 12 hours. This prevents the peak concentrations of both drugs from hitting your kidneys at the exact same time.
The most critical step is monitoring. If you start a regular NSAID regimen, your doctor should check your serum creatinine and complete blood count (CBC) within 48 to 72 hours. For those on high-dose cancer treatments, monitoring is even more intense, with blood levels checked at 24, 48, and 72 hours post-dose.
If you need a pain alternative that doesn't mess with your kidneys in the same way, consider acetaminophen (Tylenol), though keep the dose under 3 grams per day to protect your liver. For chronic inflammation, focusing on adjusting your Disease-Modifying Antirheumatic Drugs (DMARDs) to better control the disease is a safer long-term play than relying on daily NSAIDs.

The Role of Genetics and Age
Why do some people breeze through this combination while others crash? Genetics play a role. Research into the SLC19A1 gene suggests that people with a specific polymorphism (the 80G>A variant) may experience 40% more methotrexate accumulation when taking NSAIDs. This variant is present in about 15% of Caucasians, meaning a small portion of the population is naturally more vulnerable.
Age is another massive factor. Patients over 65 often have a naturally declining eGFR (estimated Glomerular Filtration Rate). Even if their kidney function seems "okay" on paper, the margin for error is much smaller. Some experts recommend absolute avoidance of NSAIDs for patients over 65 who are on methotrexate, citing a nearly three-fold increase in mortality risk in these specific groups.
Can I take a single dose of ibuprofen while on methotrexate?
For most adults with healthy kidneys and low-dose methotrexate, a single, occasional dose of ibuprofen is generally considered low risk. However, you should always check with your doctor first, as your individual kidney function (eGFR) determines whether this is safe for you.
What is the safest alternative to NSAIDs for joint pain?
Acetaminophen is typically the first alternative recommended because it does not inhibit renal prostaglandins. Other options include topical NSAIDs (which have much lower systemic absorption) or adjusting your primary DMARD therapy to better control the inflammation.
Why does my doctor check my blood so often when I start an NSAID?
They are looking for a rise in serum creatinine (a sign of kidney stress) and a drop in white blood cells or platelets. Because toxicity can be asymptomatic in the early stages, blood tests are the only way to catch a dangerous spike in methotrexate levels before it causes permanent damage.
Is celecoxib safer than ibuprofen for MTX patients?
Generally, yes. Celecoxib is a selective COX-2 inhibitor, meaning it has a smaller effect on the prostaglandins that keep the kidneys functioning. Studies show it increases methotrexate levels by about 10-15%, compared to 25-30% for ibuprofen.
What happens if methotrexate levels get too high?
Severe toxicity can lead to bone marrow suppression (leukopenia), severe mouth sores, and acute kidney failure. In critical cases, doctors use "leucovorin rescue" therapy to provide the body with the folate it needs to counteract the drug's effects.
Next Steps for Patients and Caregivers
If you're currently taking both, don't panic, but do be proactive. Start by requesting a recent eGFR test to see exactly where your kidney function stands. If your eGFR is below 60, the risk is significantly higher, and you should discuss alternative pain management with your rheumatologist immediately.
Keep a simple log of when you take your methotrexate and any over-the-counter painkillers. This helps your doctor spot patterns if your blood work starts to look off. Finally, remember that pharmacist-led reviews can reduce interaction risks by over 60%-don't be afraid to ask your pharmacist to double-check your medication list for any other potential clashes.