The ethics of mandatory vaccination policies for reemerging influenza
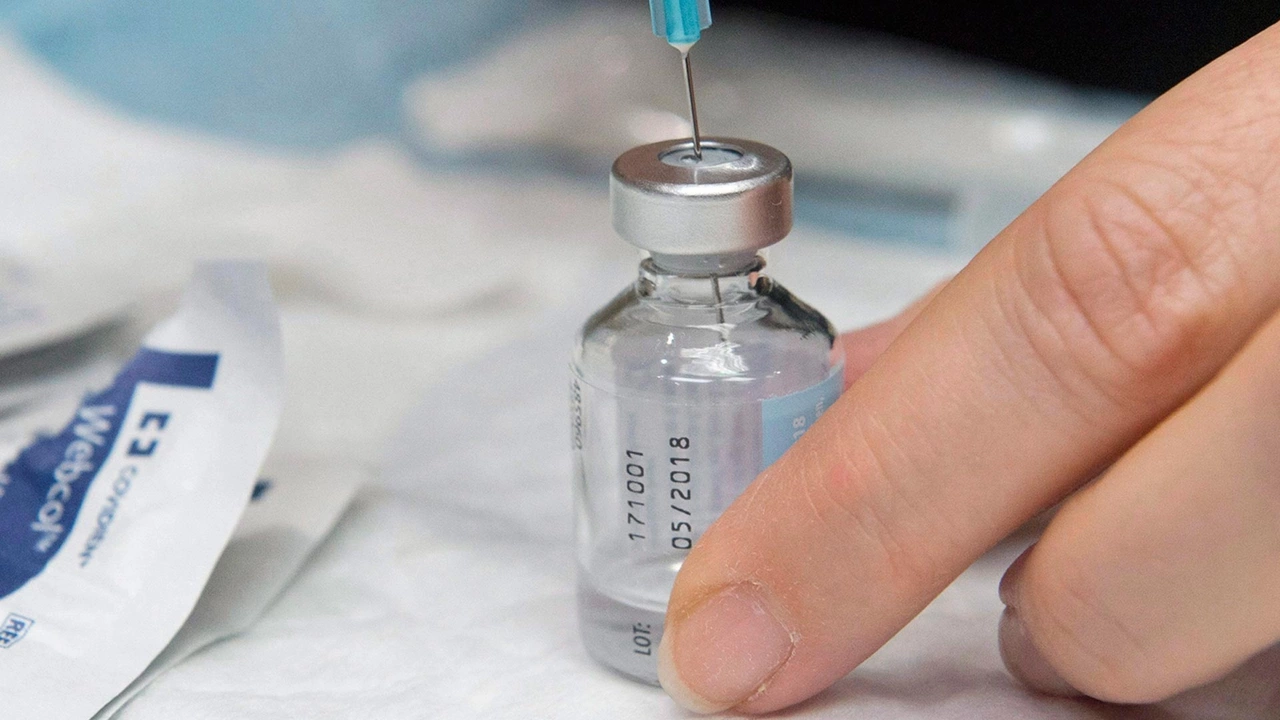
Exploring the Necessity of Mandatory Vaccination Policies
In recent years, the reemergence of influenza has sparked debates surrounding the ethics of mandatory vaccination policies. As we continue to face global health threats, it's crucial to examine the necessity of implementing such measures. This section will explore the reasons behind considering mandatory vaccinations, such as protecting vulnerable populations, achieving herd immunity, and preventing healthcare system overloads.
It's important to remember that certain groups are at a higher risk of complications from influenza, including young children, elderly individuals, and those with weakened immune systems. By enforcing mandatory vaccination policies, we can help protect these vulnerable populations and minimize the impact of the virus on their health. Additionally, achieving herd immunity is essential in stopping the spread of infectious diseases. If a large percentage of the population is immune to influenza, it becomes more difficult for the virus to spread, ultimately benefiting everyone. Lastly, preventing healthcare system overloads is another crucial factor to consider. As we've witnessed during the COVID-19 pandemic, healthcare systems can quickly become overwhelmed when dealing with large-scale outbreaks. Ensuring widespread immunity through mandatory vaccinations can help alleviate this burden.
Addressing the Ethical Concerns of Mandatory Vaccinations
While there are clear benefits to implementing mandatory vaccination policies, it's important to address the ethical concerns that arise from such measures. The primary ethical concerns include individual autonomy, informed consent, and the potential for coercion. As we delve into these issues, it's crucial to strike a balance between public health and individual rights.
Individual autonomy is a cornerstone of medical ethics, and it's important to respect a person's right to make decisions about their own body. However, in the context of public health, individual autonomy must be balanced against the collective good. Mandatory vaccination policies may infringe upon personal autonomy, but it's essential to weigh this against the potential benefits to society as a whole. Similarly, informed consent plays a significant role in ethical medical practice. Patients should be fully informed about the risks and benefits of vaccinations before making a decision. However, in cases where mandatory vaccinations are enforced, the element of choice may be diminished. Lastly, the potential for coercion is another ethical concern that must be considered. Implementing mandatory vaccination policies may lead to individuals feeling pressured to comply, even if they have reservations. It's important to ensure that these policies are implemented fairly and ethically, respecting individual rights while promoting public health.
Considering the Role of Government and Public Health Organizations
The implementation of mandatory vaccination policies raises questions about the appropriate role of government and public health organizations in enforcing such measures. In this section, we'll discuss the responsibilities of these entities in ensuring the well-being of their citizens while respecting individual rights.
Government and public health organizations have a duty to protect the health of their citizens. In the case of reemerging influenza, this may involve implementing mandatory vaccination policies. However, it's crucial for these entities to balance public health interests with individual rights. Policies should be evidence-based and designed to minimize harm, while also considering the needs of vulnerable populations. By conducting thorough research and consulting with experts, governments and public health organizations can develop fair and effective policies that prioritize public health without infringing on individual rights.
Examining Alternative Approaches to Vaccination Policies
Given the ethical concerns surrounding mandatory vaccination policies, it's important to explore alternative approaches that can promote widespread immunity without infringing on individual rights. This section will discuss strategies such as incentivizing vaccinations, improving public health education, and increasing accessibility to vaccines.
Incentivizing vaccinations can be an effective way to increase immunization rates without mandating vaccines. By offering financial incentives, discounts, or other rewards, individuals may be more likely to voluntarily receive vaccinations. Additionally, improving public health education can help dispel misinformation and increase vaccine acceptance. By providing accurate, evidence-based information about the benefits of vaccinations, individuals may be more likely to make informed decisions about their own health. Lastly, increasing accessibility to vaccines can help ensure that more people have the opportunity to receive immunizations. By offering vaccinations at convenient locations and times, and providing financial support to those in need, governments and public health organizations can encourage vaccine uptake without relying on mandatory policies.
Striking a Balance: The Future of Mandatory Vaccination Policies
In conclusion, the ethics of mandatory vaccination policies for reemerging influenza is a complex issue that requires careful consideration. While there are clear benefits to implementing such measures, it's crucial to address the ethical concerns that arise from infringing on individual rights. By striking a balance between public health and personal autonomy, we can develop fair and effective policies that protect our communities from the devastating effects of influenza.
As we continue to face global health threats, it's essential to remain vigilant and adaptable in our approach to vaccination policies. By considering alternative strategies, engaging in open dialogue, and prioritizing the well-being of our communities, we can work together to create a healthier, more resilient world for all.

Adam Stewart
I appreciate the thorough overview of the ethical landscape surrounding mandatory flu shots. The balance between protecting vulnerable groups and respecting personal autonomy is a classic public‑health dilemma. Your point about herd immunity being a communal shield really resonates with me. It’s also clear that preventing healthcare overload is not just a logistical concern but an ethical imperative. While the article lays out the arguments well, I think we could also highlight how community trust builds when policies are transparently communicated. Overall, the discussion feels both inclusive and grounded in real‑world implications.
Selena Justin
Thank you for presenting such a balanced analysis; it reflects a commendable level of scholarly rigor. The respectful tone in which you address individual autonomy demonstrates a genuine appreciation for ethical nuance. I am particularly pleased to see the emphasis on informed consent, as this upholds the dignity of each person. Moreover, your suggestions for governmental responsibility are articulated with a prudent sense of fairness. Kindly consider these reflections as an affirmation of your well‑structured argument.
Bernard Lingcod
Great to see such an energetic push for public‑health solutions without shying away from the tough ethical questions. The mixed‑formality approach makes the piece accessible yet still intellectually stimulating. I’d add that incentivizing vaccination could act as a catalyst for wider community engagement, especially when paired with clear data on efficacy. Also, the narrative could benefit from a stronger call to action for healthcare workers to lead by example. Your article already sparks a lot of momentum, and a few extra data points would make it unstoppable.
Raghav Suri
Your expert take on the policy side hits the nail on the head; aggressive implementation without proper scaffolding can backfire. At the same time, a chill, observant stance reminds us that people react best when they feel heard and not bulldozed. It would be wise to embed transparent metrics so the public can track outcomes in real time. By collaborating with community leaders, the government can soften the edge of coercion while still achieving high uptake. The balance you propose is both realistic and strategically sound.
Freddy Torres
Vaccination is the ethical quilt that stitches our collective health.
Andrew McKinnon
Ah, the classic policy‑driven prophylaxis debate-so much jargon, yet so few practical solutions in sight. While the article flaunts a respectable veneer of empathy, the undercurrent feels like a low‑grade PowerPoint lecture on risk mitigation. Let’s be honest: without genuine community buy‑in, any mandatory regime is just a bureaucratic band‑aid. The sarcasm aside, the data you cite could have been leveraged to argue for more nuanced, tiered incentives rather than blunt mandates. In short, the piece is a solid foundation, but it needs a heftier dose of street‑level realism.
Dean Gill
Reading through the comprehensive exposition, I am struck by how intricately you have woven together the threads of legal precedent, epidemiological data, and philosophical doctrine into a tapestry that both informs and provokes. The opening sections adeptly foreground the vulnerable cohorts-children, the elderly, immunocompromised individuals-illustrating the undeniable moral imperative to shield those who cannot protect themselves. Your discussion of herd immunity rightly acknowledges that it is not merely a statistical abstraction but a lived reality that can avert catastrophic healthcare system overloads, as starkly demonstrated during recent pandemics. Moreover, the ethical critique of individual autonomy is handled with a nuance that respects personal sovereignty while recognizing the collective stakes at play. When you transition to the role of government, the argument that evidence‑based policies must be balanced against civil liberties resonates with the foundational principles of liberal democracy. The alternative strategies you propose-financial incentives, robust public education, and expanded vaccine access-are not only pragmatic but also align with empowerment models that avoid coercion. What I find especially compelling is your call for a dynamic, adaptable framework that can evolve as viral patterns shift, thereby ensuring that the policy ecosystem remains both resilient and ethically sound. In emphasizing dialogue and transparency, you set the stage for a societal consensus that can transcend partisan divides. The piece, therefore, stands as a model for how public health discourse can be both scientifically rigorous and morally attentive. It invites policymakers, clinicians, and citizens alike to reflect deeply on the trade‑offs inherent in any health intervention. Ultimately, your conclusion-that a balanced, collaborative approach can forge a healthier, more resilient world-offers both hope and a concrete roadmap for future action. This synthesis of ethical theory and actionable policy is precisely the kind of scholarship that can drive meaningful change.